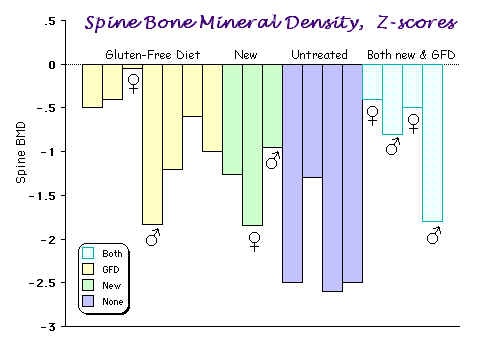
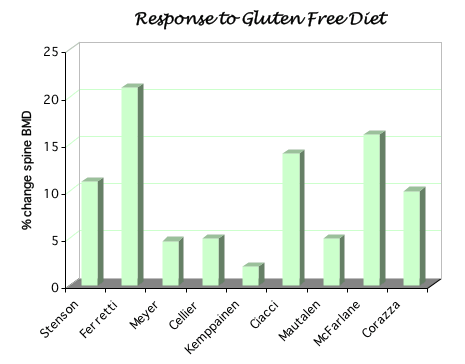
The graph shows results from several studies showing generally low bone densities in patients, which are somewhat better when they are on a gluten-free diet. Click to see a table with some details from these studies.
Celiac sprue is an intestinal disease associated with insensitivity to glutens. There is a wide spectrum of manifestations, from serious diarrhea in infants when they start eating cereals to completely asymptomatic patients discovered by studies of prevalence. About 1% of white Americans and Europeans have sprue. Most patients have at least some gastrointestinal symptoms. Calcium and iron are the most difficult nutrients to absorb, so these patients freqently have osteoporosis or anemia. The disease may be inherited but no specific gene has been identified.

The graph shows results from several studies showing generally low bone densities in patients, which are somewhat better when they are on a gluten-free diet. Click to see a table with some details from these studies.
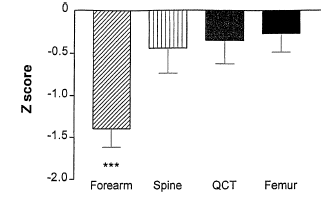
Selby PL et al. Bone loss in celiac disease is related to secondary hyperparathyroidism. J Bone Miner Res. 1999;14(4):652-7.
This shows results from one study of patients with low bone density at the forearm depsite a gluten-free diet.
Patients with celiac sprue may have low 25-hydroxy-vitamin D, but they can have osteoporosis and calcium malabsorption even with normal levels. The 1,25-dihydroxyvitamin D levels are frequently elevated and are not the correct test to determine vitamin D status. Hypocalcemia can be seen but usually the serum calcium is normal.
The 24-hour urine calcium is characteristically low in these patients.
Several papers have found evidence of secondary hyperparathyroidism, which is probably one of the pathophysiological mechanisms for the osteoporosis, as shown in the following figure:
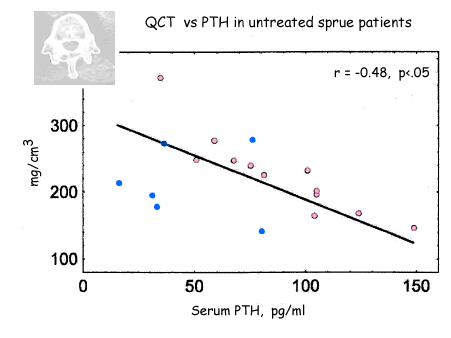
Ferretti J et al. Analysis of the structure and strength of bones in celiac disease patients. Am J Gastroenterol. 2003;98(2):382-90. Blue dots:men; pink dots:women
New tests for sprue include IgA antibodies against endomysial and against tissue transglutaminase. These tests are felt to have high sensitivity (about 95%) and specificity (about 98 to 99%) for celiac sprue. The diagnosis is confirmed with a small bowel biopsy. It is wise to confirm the diagnosis because a gluten-free diet is a major change in life-style and should not be recommended unless sprue is definitely present.
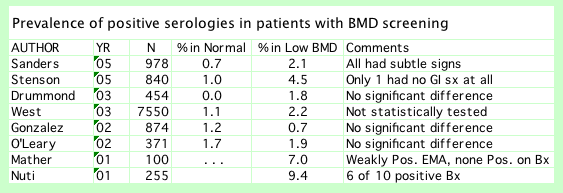
The following table shows results of studies that have measured the antibodies in patients screened for bone density. Although the patients with osteoporosis have a higher chance of having sprue, the incidence is still low enough that routine screening is not cost-effective. Besides, the largest studies found that most of the patients who had osteoporosis as well as sprue had subtle gastrointestinal symptoms.
If a patient has osteoporosis without other explanation, especially if the bone density is lower than expected for age, then these tests should be considered.
Stenson and colleagues discovered 8 cases of unrecognized celiac sprue who had osteoporosis. These patients had all failed to respond to alendronate. Following a gluten-free diet, these patients showed improvement: 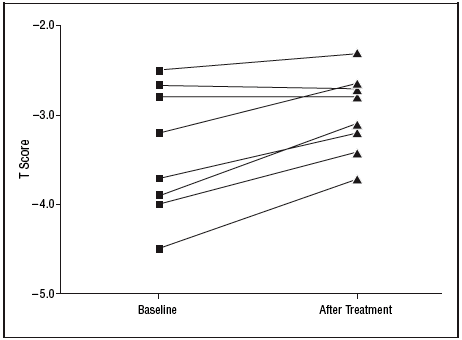
Stenson WF et al, Increased prevalence of celiac disease and need for routine screening among patients with osteoporosis. Arch Intern Med. 2005;165(4):393-9.
Recently Pazianas et al studied calcium absorption in patients who had received an average of 4 years treatment with a gluten-free diet, but they still had decreased calcium absorpion. The vitamin D and PTH levels were normal, but the PTH was inversely correlated with the bone density. Patients with celiac sprue require greater calcium intake than normals (2,000mg/day). There is good rationnale for giving calcitriol to these patients, but this has not been studied.

