More about Vitamin D
Active metabolites of vitamin D
Metabolites of vitamin D increase the intestinal absorption of calcium. These steroid hormones have many other cellular effects, such as increasing the differentiation of cells and stimulating pre-osteoclasts. Calcitriol (1,25 (OH)2 vitamin D, the most active metabolite) increases osteocalcin production by osteoblasts and thus has been considered to stimulate bone formation. Several studies, however, have shown that calcitriol does not increase the bone formation rate measured directly from bone biopsies.
Active metabolites of vitamin D have been advocated for treatment of osteoporosis. A common misunderstanding is that calcitriol has a dose-dependent effect on bone mass. Studies of populations with vitamin D deficiency or poor calcium nutrition show improvement in bone mass, but this is not seen in women who are well nourished. In the U.S. three studies of calcitriol all showed no significant increase in bone mass compared to baseline, although the two smaller studies showed the calcitriol group had better change in bone density than the placebo group in some skeletal areas.
Researchers from New Zealand concluded that calcitriol treatment reduced the rate of vertebral fractures. This unblinded study had a 30% drop-out rate which might have biased the results. Bone mass was not measured.
Here is a
table of clinical trials using calcitriol for postmenopausal osteoporosis
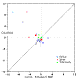 This graph shows controlled trials that reported bone density in each group. The results of the controls are plotted vs the results of the treated subjects, so that the points that fall ABOVE the diagonal line represent studies in which the treatment group was BETTER than the control group. The size of the point is proportional to the nubmer of subjects in the study.
This graph shows controlled trials that reported bone density in each group. The results of the controls are plotted vs the results of the treated subjects, so that the points that fall ABOVE the diagonal line represent studies in which the treatment group was BETTER than the control group. The size of the point is proportional to the nubmer of subjects in the study.
Calcitriol is not a benign drug. Virtually every study has shown dramatic increases in the urine calcium levels. Long-term use could potentially be damaging to the kidney. The early studies of calcitriol or 1a-hydroxy vitamin D are replete with examples of serious hypercalcemia, some requiring hospitalization.
Calcitriol should not be recommended for the patient with idiopathic postmenopausal osteoporosis because it does not usually improve bone mass in patients who have adequate calcium and vitamin D levels, and because it has an unacceptable risk/benefit ratio. Hypercalcemia and hypercalciuria are frequently reported. However, calcitriol is beneficial in patients who have mild intestinal malabsorption, and may be a useful adjuvant therapy in cases of steroid-induced osteoporosis. In cases of moderate renal failure with evidence of parathyroid stimulation, calcitriol can prevent the development of "tertiary" hyperparathyroidism. These patients must be monitored carefully, with attention paid to the calcium intake and the urine calcium.
Vitamin D disorders
High levels of vitamin D are usually iatrogenic, resulting in hypercalcemia and/or hypercalciuria. Some patients with kidney stones have slightly high 1,25 (OH)2D levels, with increased intestinal absorption of calcium but normal serum calcium. Granulomatous diseases or lymphomas may also produce excess 1,25 (OH)2D, and patients with primary hyperparathryoidism have slightly increased levels.
Vitamin D deficiency is seen in patients with inadequate sunlight exposure who also ingest inadequate amounts of vitamin D. Examples are nursing home patients, breast-fed babies who don't get outside, Arabian women who move to London. Patients with malabsorption also may have vitamin D deficiency.
Liver disease can result in low levels of 25-hydroxy-vitamin D, but usually this does not happen until end-stage liver failure. Renal disease results in decreased levels of 1,25 (OH)2D. The levels gradually decrease in parallel to decreases in renal function, and by the time patients require dialysis they virtually always have calcium abnormalities.
A very rare but fascinating disorder is oncogenic osteomalacia, in which a mesenchymal tumor secretes a factor ("phosphatonin", which is FGF23 in many cases) which acts on the renal tubule to inhibit vitamin D and to increase urine phosphate loss. Other rare disorders include inborn errors of metabolism, such as lack of vitamin D receptor (Vitamin D resistance) or lack of the renal 1-alpha-hydroxylase.
These deficiency disorders may all eventually cause osteomalacia. Photomicrographs of osteomalacia and secondary hyperparathryoidism caused by renal failure can be found in the gallery.
Other effects
Vitamin D has many other effects that are somewhat beyond this web site. They include:
Treating psoriasis
Inhibiting proliferation of cancer cells
Modulating infections and immune function
Providing some protection against diabetes and multiple sclerosis
Improving muscle strength
 Two new systematic reviews of vitamin D and cardiovascular disease were published in the March 2010 Annals of Internal Medicine (not in PubMed yet). Both found no overall significant benefit from vitamin D supplementation, and suggest that further randomized trials should be done before recommending vitamin D supplementation to the general public.
Two new systematic reviews of vitamin D and cardiovascular disease were published in the March 2010 Annals of Internal Medicine (not in PubMed yet). Both found no overall significant benefit from vitamin D supplementation, and suggest that further randomized trials should be done before recommending vitamin D supplementation to the general public.
Lu Wang, MD, PhD; JoAnn E. Manson, MD, DrPH; Yiqing Song, MD, ScD; and Howard D. Sesso, ScD. Systematic Review: Vitamin D and Calcium Supplementation in
Prevention of Cardiovascular Events
Anastassios G. Pittas, MD, MS; Mei Chung, MPH; Thomas Trikalinos, MD; Joanna Mitri, MD; Michael Brendel, BA; Kamal Patel, MPH;
Alice H. Lichtenstein, DSc; Joseph Lau, MD; and Ethan M. Balk, MD, MPH. Systematic Review: Vitamin D and Cardiometabolic Outcomes.
Updated 3/2/10


 This graph shows controlled trials that reported bone density in each group. The results of the controls are plotted vs the results of the treated subjects, so that the points that fall ABOVE the diagonal line represent studies in which the treatment group was BETTER than the control group. The size of the point is proportional to the nubmer of subjects in the study.
This graph shows controlled trials that reported bone density in each group. The results of the controls are plotted vs the results of the treated subjects, so that the points that fall ABOVE the diagonal line represent studies in which the treatment group was BETTER than the control group. The size of the point is proportional to the nubmer of subjects in the study.
 Two new systematic reviews of vitamin D and cardiovascular disease were published in the March 2010 Annals of Internal Medicine (not in PubMed yet). Both found no overall significant benefit from vitamin D supplementation, and suggest that further randomized trials should be done before recommending vitamin D supplementation to the general public.
Two new systematic reviews of vitamin D and cardiovascular disease were published in the March 2010 Annals of Internal Medicine (not in PubMed yet). Both found no overall significant benefit from vitamin D supplementation, and suggest that further randomized trials should be done before recommending vitamin D supplementation to the general public.
