
Calories and the importance of weight
Alcohol: Avoid excess
Calcium
Vitamin D
Protein: Good for your bones
Vitamin A: Avoid excess
Vitamin K
Caffeine
Magnesium
Acid load
Other
 |
Calories and the importance of weight Alcohol: Avoid excess Calcium Vitamin D Protein: Good for your bones Vitamin A: Avoid excess Vitamin K Caffeine Magnesium Acid load Other |
|
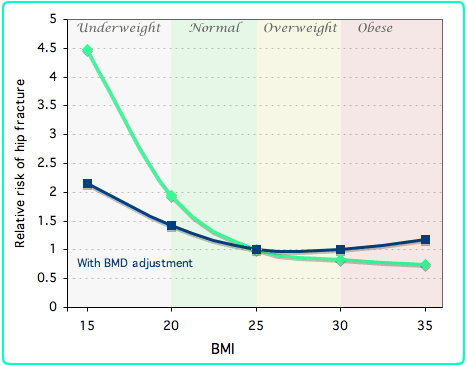
Use this to calculate your BMI (Body Mass Index) |
The meta-analyses of 60,000 men and women throughout the world documented that low body mass index (BMI) is an important risk factor for hip fractures as well as all kinds of osteoporotic fractures (De Laet). Notice that the risk of a hip fracture is twice as high in somebody with a BMI of 20 compared to somebody with a BMI of 25. Some of this is caused by decreased bone density, but even when adjusted for bone density (as shown in the dark blue line) there is an increased fracture risk with low weight.
The baseline data from Study of Osteoporotic Fractures showed that weight gain since the age of 25 was associated with a lower risk of fracture. These women, who were older than 65, were then followed for 4 years and those who lost more than 5% of weight had more than twice the number of hip fractures as those who did not lose weight. This was true even if they were overeweight and voluntarily lost the weight (Ensrud KE).
Salamone showed that women in a weight-reduction study assigned to the intervention group lost an average of 3.2kg, but they lost bone density twice as fast as those who were in the weight-stable control group. Weight loss was the strongest predictor for bone loss seen in men and women from Rancho Bernardo (Knoke). The bone resorption markers are better during weight loss when a high protein-high calcium-low calorie diet is used to lose weight (Bowen), so this might help reduce the fracture risk.
The importance of weight is not emphasized very much, but study after study shows that weight is a stronger risk factor than calcium or other nutrients.
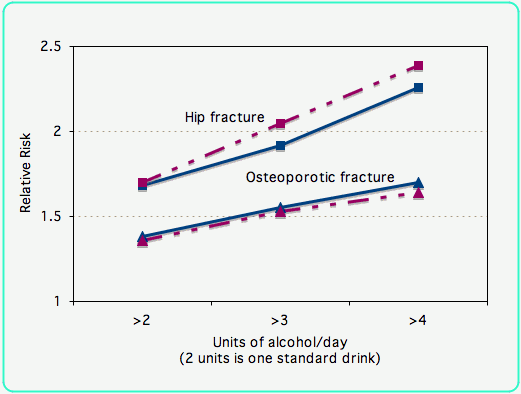
 This is data from an international meta-analysis on the effect of alcohol on fracture rates in 16,971 men and women. For hip fractures the relative risk was greater when adjusting for the bone density (shown in the dashed line), because alcohol increases bone density as well as fracture risk. The risks are shown comparing those who drink more than 2, 3 or 4 units of alcohol with those drinking less than that amount. One unit of alcohol is 8 grams. A "standard drink" is 14 grams, corresponding to a glass of wine, can of beer or a jigger of spirits
(Kanis JA).
This is data from an international meta-analysis on the effect of alcohol on fracture rates in 16,971 men and women. For hip fractures the relative risk was greater when adjusting for the bone density (shown in the dashed line), because alcohol increases bone density as well as fracture risk. The risks are shown comparing those who drink more than 2, 3 or 4 units of alcohol with those drinking less than that amount. One unit of alcohol is 8 grams. A "standard drink" is 14 grams, corresponding to a glass of wine, can of beer or a jigger of spirits
(Kanis JA).
Alcohol in small amounts is slightly beneficial to the bone; those who consume 1 unit a day (2 or 3 drinks a week) had higher bone density and a lower fracture rate than teetotallers. Between 1 and 2 units a day there is no increased risk. But above that amount the risk starts climbing.
Alcohol increases aromatase activity and the benefits with small amounts might be related to the higher levels of estrogens in both men and women.
 These are discussed on separate pages.
These are discussed on separate pages.

Most of the largest studies find a benefit of protein on the bone. The Framingham study of bone loss over 4 yrs in 614 elderly men and women showed more bone loss in those with lower animal protein intake, even when adjusting for multiple other factors (Hannan).
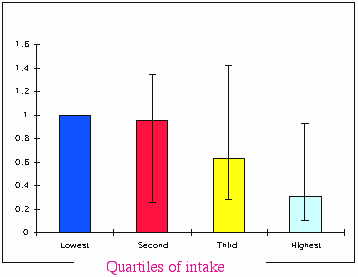 | Risk of hip fracture according to animal protein intake in postmenopausal women. In this study of 104338 person-years, the multivariate model (which included body size) found lower fracture rates in those with highest protein intakes (Munger). |
In another study of elderly people, animal protein intake was associated with protection from bone loss (Promislow JH). There was one study, however, that suggested that a high ratio of animal to vegetable protein increased the rate of bone loss (Sellmeyer).
A placebo controlled trial of protein supplement (dairy-based) in patients with recent hip fracture showed attenuated bone loss in the femur (Schurch).
High protein diets cause increase in urine calcium, but this is because there is more calcium absorbed from the intestines. Also, amino acids can increase the glomerular filtration rate which can increase urine calcium. The calcium resorbed from the bones is actually decreased with high protein intake (Kerstetter).
|
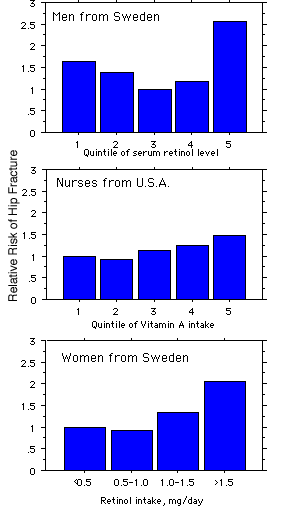
Four recent studies have shown that excess vitamin A is harmful to bones. One showed decreased bone density with both vitamin A excess and deficiency (Promislow, J. H.). The other three show increases in hip fracture rates, as shown in the graph. (Feskanich, D.,
Melhus, H.,
Michaelsson, K.).
For the purposes of food labels, the daily value = 5000 IU per day. The Institute of Medicine recommendation, however, is 2330 IU = 700 micrograms (for women) and 3000 IU = 900 micrograms (for men). One microgram of vitamin A (retinol) = 3.33 international units. Each 12 micrograms of beta-carotene from dietary sources is equal to 1 microgram of vitamin A retinol. If beta-carotene is taken as a supplement in oil, then each 2 micrograms is equal to 1 microgram of vitamin A. More reference data from the NIH. Here is a link to a long review by the Institute of Medicine. |

Vitamin K deficiency prevents carboxylation of gla-proteins, including osteocalcin. Several studies show inverse relationship between decarboxylated osteocalcin and bone density. The Nurses Health Study showed women with vitamin K intakes in lowest quintile (<109 �g/d) had increased risk of hip fracture. The Framingham study did not show any relationship between vitamin K intake and BMD or hip fracture, and the Study of Osteoporotic Fractures showed reduced hip fractures in women with high lutein intake, which is related to vitamin K.
Reports about Vitamin K supplements show some conflicts. One study suggested that vitamin K supplements may reduce the rate of bone loss in women aged 50-60 (Braam LA) but another large nested case-control study found no relationship between vitamin K intake and fractures in that age range (Rejnmark L).
Coffee has small effects on the bone and on calcium. One cup of coffee decreases calcium balance by about 6mg - less than the amount of calcium in a tablespoon of milk! Most of the loss is due to a slight decrease in the gastrointestinal absorption of calcium (Barger-Lux MJ). Overall, caffeine does not cause serious problems with calcium economy (Heaney RP, Hasling C).
The Framingham study found no increase in fracture risk with 2 cups of coffee or 4 cups of tea daily, but above that the risk of fracture increased (Kiel DP). The Study of Osteoporotic Fractures also found a 20% increased risk of hip fractures in elderly women who drank more than 190 mg of caffeine (about 2 cups) daily (Cummings SR).
Fortunately, drinking milk can cancel effects of caffeine on calcium metabolism (Barrett-Connor E). Therefore, you come out ahead with a latte or a mocha!
There is a lot of advertising and very little real data about the effects of magnesium on the skeleton. Magnesium deficiency causes hypocalcemia and hyperparathyroidism (at moderately low levels) or hypoparathyroidism (at seriously low levels). Magnesium deficiency is seem with some medications and with alcoholism, malabsorption, or malnutrition.
A small study showed no effect on biochemical markers after one month of Mg supplementation in young women. In adolescent girls, dietary Mg was inversely associated with BMD, whereas calcium intake was positively associated with BMD. A frequently referenced study showing benefit of Mg in women with osteoporosis compared calcium-Mg supplement to control group who were given placebo and told to limit dairy intake, so of course the women taking calcium and magnesium had a better bone density response. A recent study suggested bone density might increase with magnesium.
A presentation at the 2002 ABSMR meetings from the Women's Health Initiative showed that dietary magnesium intake DID NOT prevent fractures. The women who consumed the most magnesium had the highest rate of wrist and lower arm fractures.
Therefore, more careful studies are needed before supplementation can be advised. Magnesium might compete with calcium. It alter the crystals within the bones but the effect of that is uncertain.
Magnesium is present in a normal healthy diet, especially in dark green vegetables and nuts.
It is well known that renal tubular acidosis causes bone disease. Perhaps subtle forms of renal acidosis could contribute to postmenopausal osteoporosis. Metabolic alkalosis seems to be good for the bone.
Fruits and vegetables contain alkali which is associated with improved bone density. During the menopausal transition, fruits and vegetables seem to help prevent some of the bone loss. This might be due to the alkali and/or potassium in these foods (Macdonald HM)
Some studies have found beneficial effects of potassium citrate. I am planning to include these on this web page.

