Because this is a relatively new procedure, there is little information about the bone disease in these patients. However available studies have shown fracture rates of 15 to 45%, and bone density is frequently low. Diabetes itself may contribute to low bone formation rate, but patients who have high body mass index tend to have high bone density. After transplantation, acidosis may complicate the bone disease. Also, diabetic neuropathy enhances the likelihood of stress fractures in the feet and ankles, which account for a large proportion of the fractures in this group of patients.
References
Almond, M. K.(1994). Loss of regional bone mineral density in the first 12 months following renal transplantation. Nephron 66(1): 52-7.
Aroldi, A.(1997). Effects of three immunosuppressive regimens on vertebral bone density in renal transplant recipients: a prospective study. Transplantation 63(3): 380-6.
Bagni, B.(1994). Continuing loss of vertebral mineral density in renal transplant recipients. Eur J Nucl Med 21(2): 108-12.
Bardin, T.(1995). Dialysis arthropathy: outcome after renal transplantation [see comments]. Am J Med 99(3): 243-8.
Behnke, B.(1996). Bone mineral density in pediatric patients after renal transplantation. Clin Nephrol 46(1): 24-9.
Berenson, J. R.(1997). Pharmacokinetics of pamidronate disodium in patients with cancer with normal or impaired renal function. J Clin Pharmacol 37(4): 285-90.
Boot, A. M.(1995). Renal transplantation and osteoporosis. Arch Dis Child 72(6): 502-6.
Braun, W. E.(1999). The incidence and management of osteoporosis, gout, and avascular necrosis in recipients of renal allografts functioning more than 20 years (Level 5A) treated with prednisone and azathioprine. Transplantation Proceedings 31(1-2): 1366-1369.
Briner, V. A.(1995). Prevention of cancellous bone loss but persistence of renal bone disease despite normal 1,25 vitamin D levels two years after kidney transplantation. Transplantation 59(10): 1393-400.
Chao, S. H.(1994). Bone mineral density profile in uremic and renal transplant patients. Transplant Proc 26(4): 2009-11.
Cueto-Manzano, A. M.(1999). Bone loss in long-term renal transplantation: histopathology and densitometry analysis [In Process Citation]. Kidney Int 55(5): 2021-9.
Davenport, A.(1993). Treatment of hypercalcaemia with pamidronate in patients with end stage renal failure. Scand J Urol Nephrol 27(4): 447-51.
David-Neto, E.(1993). Reversal of aluminum-related bone disease after renal transplantation. Am J Nephrol 13(1): 12-7.
Dissanayake, I. R.(1998). The fate of bone after renal transplantation. Current Opinion in Nephrology and Hypertension 7(4): 389-395.
Elmstedt, E.(1981). Avascular bone necrosis in the renal transplant patient: a discriminant analysis of 144 cases. Clin Orthop(158): 149-57.
Elmstedt, E.(1982). Incidence of skeletal complications in renal graft recipients. Effect of changes in pharmacotherapy. Acta Orthop Scand 53(6): 853-6.
Elmstedt, E.(1982). Spontaneous fractures in the renal graft recipient: a discriminant analysis of 144 cases. Clin Orthop(162): 195-201.
Feber, J.(1994). Bone mineral density after renal transplantation in children. J Pediatr 125(6 Pt 1): 870-5.
Grotz, W. H.(1994). Bone fracture and osteodensitometry with dual energy X-ray absorptiometry in kidney transplant recipients. Transplantation 58(8): 912-5.
Grotz, W. H.(1995). Bone loss after kidney transplantation: a longitudinal study in 115 graft recipients. Nephrol Dial Transplant 10(11): 2096-100.
Grotz, W. H.(1995). Bone mineral density after kidney transplantation. A cross-sectional study in 190 graft recipients up to 20 years after transplantation. Transplantation 59(7): 982-6.
Grotz, W. H.(1998). Treatment of osteopenia and osteoporosis after kidney transplantation. Transplantation 66(8): 1004-8.
Grotz, W.(1998). Treatment of bone pain after kidney transplantation. Transplant Proc 30(5): 2114-6.
Horber, F. F.(1994). Changes in bone mass early after kidney transplantation. J Bone Miner Res 9(1): 1-9.
Hung, C. J.(1996). Clinical implication of hormone treatment in postmenopausal kidney transplants. Transplant Proc 28(3): 1548-50.
Hurst, G.(1998). Stabilization of bone mass after renal transplant with preemptive care. Transplant Proc 30(4): 1327-8.
Isiklar, I.(1998). Changes in bone mineral density after renal transplantation. Transplant Proc 30(3): 814-5.
Julian, B. A.(1991). Rapid loss of vertebral mineral density after renal transplantation. N Engl J Med 325(8): 544-50.
Kalef-Ezra, J. A.(1994). Bone mineral status after renal transplantation. Assessment by noninvasive techniques. Invest Radiol 29(2): 127-33.
Kim, M. S.(1998). Effect of deflazacort on bone mineral density in renal transplant recipients. Transplant Proc 30(7): 3041-2.
Kim, H.(1998). Bone mineral density after renal transplantation. Transplant Proc 30(7): 3029-30.
Klaus, G.(1998). Weight-/height-related bone mineral density is not reduced after renal transplantation. Pediatr Nephrol 12(5): 343-8.
Kwan, J. T.(1992). Changes in total body bone mineral content and regional bone mineral density in renal patients following renal transplantation. Miner Electrolyte Metab 18(2-5): 166-8.
Lausten, G. S.(1998). Necrosis of the femoral head after kidney transplantation. Clinical Transplantation 12(6): 572-574.
Lindsay, R.(1976). The value of bone density measurements in predicting the risk of developing avascular necrosis following renal transplantation. Calcif Tissue Res 21 Suppl: 242-6.
Lippuner, K.(1998). Effects of deflazacort versus prednisone on bone mass, body composition, and lipid profile: a randomized, double blind study in kidney transplant patients. J Clin Endocrinol Metab 83(11): 3795-802.
Machado, C. E.(1996). Safety of pamidronate in patients with renal failure and hypercalcemia. Clin Nephrol 45(3): 175-9.
Massari, P. U.(1997). Disorders of bone and mineral metabolism after renal transplantation. Kidney International 52(5): 1412-1421.
McIntyre, H. D.(1995). Long-term bone loss after renal transplantation: comparison of immunosuppressive regimens. Clin Transplant 9(1): 20-4.
Messa, P.(1998). Persistent secondary hyperparathyroidism after renal transplantation. Kidney Int 54(5): 1704-13.
Moore, L. W.(1996). Clinical observations of metabolic changes occurring in renal transplant recipients receiving ketoconazole. Transplantation 61(4): 537-41.
Pichette, V.(1996). Long-term bone loss in kidney transplant recipients: a cross-sectional and longitudinal study. Am J Kidney Dis 28(1): 105-14.
Ramsey-Goldman, R.(1999). Increased risk of fracture in patients receiving solid organ transplants. Journal of Bone and Mineral Research 14(3): 456-463.
Sanchez, C. P.(1998). Bone disease in children and adolescents undergoing successful renal transplantation. Kidney Int 53(5): 1358-64.
Sellers, E.(1998). The use of pamidronate in three children with renal disease. Pediatr Nephrol 12(9): 778-81.
Setterberg, L.(1996). Bone demineralization after renal transplantation: Contribution of secondary hyperparathyroidism manifested by hypercalcaemia. Nephrology Dialysis Transplantation 11(9): 1825-1828.
Smets, Y. F.(1998). Low bone mass and high incidence of fractures after successful simultaneous pancreas-kidney transplantation. Nephrol Dial Transplant 13(5): 1250-5.
Smets, Y. F.(1998). Pattern of bone loss after simultaneous pancreas-kidney transplantation: a prospective study. Transplant Proc 30(2): 326.
Svahn, T.(1975). Avascular necrosis of the bone in 99 renal allograft recipients. Scand J Urol Nephrol(29 Suppl): 135-7.
Talalaj, M.(1996). Efficiency of preventive treatment of glucocorticoid-induced osteoporosis with 25-hydroxyvitamin D3 and calcium in kidney transplant patients. Transplant Proc 28(6): 3485-7.
Torregrosa, J. V.(1995). Factors involved in the loss of bone mineral density after renal transplantation. Transplant Proc 27(4): 2224-5.
Torregrosa, J. V.(1995). Evolution of bone mineral density after renal transplantation: related factors. Nephrol Dial Transplant 10 Suppl 6: 111-3.
Tyrrell, C. J.(1994). Intravenous pamidronate: infusion rate and safety. Ann Oncol 5 Suppl 7: S27-9.
Valimaki, M. J.(1999). A prospective study of bone loss and turnover after allogeneic bone marrow transplantation: effect of calcium supplementation with or without calcitonin. Bone Marrow Transplantation 23(4): 355-361.
Velasquez-Forero, F.(1996). Adynamic bone lesion in renal transplant recipients with normal renal function. Nephrol Dial Transplant 11 Suppl 3: 58-64.
Wolpaw, T.(1994). Factors influencing vertebral bone density after renal transplantation. Transplantation 58(11): 1186-9.
Yap, A. S.(1990). Use of aminohydroxypropylidene bisphosphonate (AHPrBP, "APD") for the treatment of hypercalcemia in patients with renal impairment [see comments]. Clin Nephrol 34(5): 225-9.
Yazawa, K.(1998). Positive effects of kidney transplantation on bone mass. Transplant Proc 30(7): 3031-3.
| BACK to Transplant bone disease | FORWARD to Liver transplant |
.
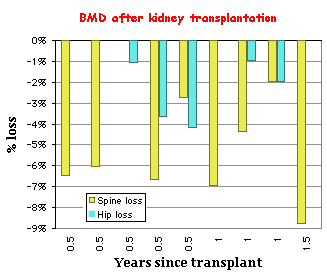 Bone density decreases in patients after renal transplantation, although there is some variation in reported rates of loss. This may reflect the underlying variability in types of renal osteodystrophy that exist prior to transplantation. Ongoing studies suggest that the rate of loss is greatest in the first year, but after several years the rate of loss is about 1-2%/year.
Bone density decreases in patients after renal transplantation, although there is some variation in reported rates of loss. This may reflect the underlying variability in types of renal osteodystrophy that exist prior to transplantation. Ongoing studies suggest that the rate of loss is greatest in the first year, but after several years the rate of loss is about 1-2%/year.