The statin story seemed to start with a report by Greg Mundy which showed increased bone morphogenic protein (BMP) in cells exposed to statins. But previous studies had shown the importance of the mevalonate pathway in bone resorption, in the context of explaining the actions of the aminobisphosphonates. Clinical investigators have been scrambling to study the effects in human subjects, and these reports are both interesting and conflicting. On this page I will present the clinical papers first, then the background scientific studies about this important aspect of bone physiology.
Published studies of clinical effects of statins
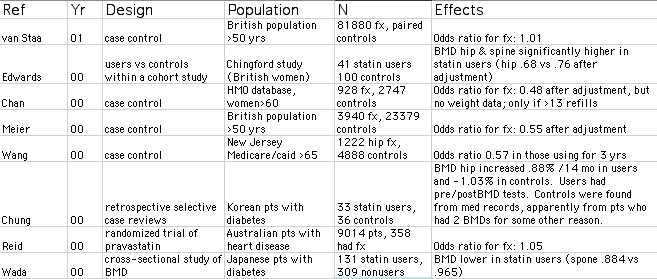
Unpublished studies
The group of investigators from San Francisco, which has a coordinating center for several large osteoporosis studies, analyzed data from three of the large studies (SOF, FIT, and HERS). They reported that women who were taking statins for high cholesterol had a reduced rate of fracture. The bone density was modestly increased as well. Most of the women were taking lovastatin. This was presented as an abstract at the 1999 meetings of the ASBMR.
At the 2000 ASBMR meetings, two abstracts from the Women's Health Initiative were presented:
J. Cauley et al: Statin Use and Bone Mineral Density (BMD) in Older Women: The Women's Health Initiative Observational Study (WHI-OS)
-
In 6,442 women enrolled in the WHI-OS at the three BMD clinical sites; 422 (6.5%) reported statin use at baseline (1993-97). Statin users tended to be older than non-users (65.9 and 63.6 years, respectively). Current hormone use was reported by 42% of users and 46% of non-users. Age and BMI adjusted total hip BMD was significantly higher among users (0.86 g/cm2) compared to non-users (0.84 g/cm2), p=0.02, but there was no difference in total body or lumbar spine BMD. We conclude that longer duration of statins and high statin potency may have modest protective effects on hip BMD in older women.
Comment: This was in the abstract book, but the oral presentation suggested that statins did not significantly improve bone density after adjustment for other known risk factors.
LaCroix, AC: Does Statin Use Reduce Risk of Fracture in Postmenopausal Women? Results from the Women's Health Initiative Observational Study (WHI-OS)
-
In the Women's Health Initiative Observational Study (WHI-OS) of postmenopausal women aged 50-79 years, we compared rates of hip, lower arm or wrist, and other clinical fractures among 7847 current statin users at baseline to rates in 85,876 non-users. 187 hip fractures, 1047 lower arm/wrist fractures and 4041 other fractures occurred. Rates of hip fracture were similar among statin users (1.07/1000 person-years) and non-users (0.83/1000 person-years). Longer duration of use (>3 years) was not significantly associated with fracture risk compared to non-users. Findings were similar for the individual statin agents examined separately. These findings do not indicate that use of currently marketed statin medications has an impact on reducing risk of osteoporotic fracture in the large WHI-OS cohort.
Background scientific studies
Trying to understand effects of inhibitors of protein prenylation, Luckman, S. P.along with Rogers and Graham Russell and colleagues, examined effects of mevastatin on prenylation of GTP-binding proteins. They showed that mevastatin caused apoptosis of murine osteoclasts in vitro.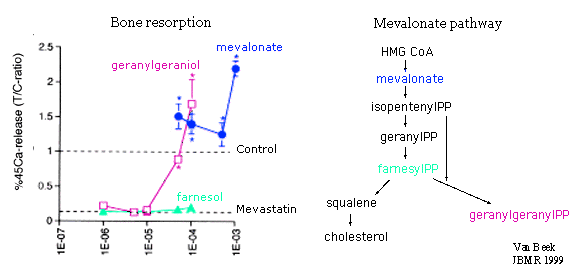
These findings were confirmed by studies from the Netherlands by van beek, E. and Papapoulos et al, as shown in the above. Mevastatin suppressed osteoclastic resorption with doses that, on a molar basis, were similar to those of the potent bisphosphonate ibandronate. When mevalonate or geranylgeraniol were added, the inhibition was reversed. These results were compared to those of bisphosphonates. Osteoclast activity is restored by mevalonate when inhibited by statins (but not when inhibited by bisphosphonates), and by geranylgeranyl pyrophosphate when inhibited by either.
GeranylgeranylPP modifies (prenylates) a small GTP-binding protein called rho21, which regulates the cytoskeleton. Thus, inhibition of geranlygeranylPP leads to abnormalies in the cytoskeleton, so osteoclasts don't have a ruffled border and are unable to resorb bone.
Meanwhile, . . .
Mundy, G. and colleagues demonstrated that statins increase production of one of the important bone growth factors (bone morphogenic protein, or BMP), which directly stimulates osteoblast activity and bone formation. When applied to mouse calvaria or given orally to rats, bone formation and bone density increased.In other studies, statins have been shown to increase bone mass. Furthermore, there is a wide range of potencies in the ability of different statins to stimulate BMD production (Sugiyama, M ), with cerivastatin showing effects an order of magnitude stronger than other statins (Garrett, I. R., ASBMR abstract)
Thus, studies from animals and cell cultures suggest that statins could have two different effects on the bone: to block the osteoclasts and to stimulate the osteoblasts. If this were true, they would be the only known drugs to have both actions.