
Mechanical Ventilation
Case 3
A patient is admitted to the ICU with severe necrotizing pancreatitis. A few hours after admission, he developed increasing oxygen requirements and was intubated for hypoxemic respiratory failure. Initially, his oxygen saturations improved to the mid-90% range on an FIO2 of 0.5, but in the past 2 hours, the nurse has had to increase the FIO2 back to 0.7 and his SaO2 is still in the lower 90% range. The patient remains on a PEEP of 5 cm H2O. The nurse drew an ABG which shows pH 7.35, pCO2 38, PO2 60, HCO3- 22 on an FIO2 of 0.8. The patient’s repeat chest x-ray is shown below. An echocardiogram performed earlier in the day revealed normal left ventricular function.
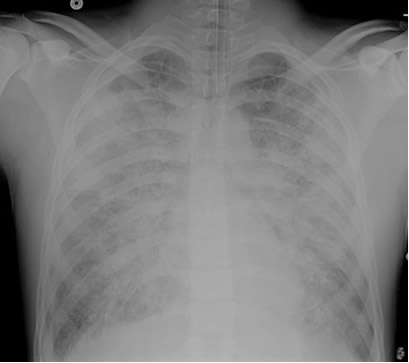
How do you explain his worsening oxygenation status?
What can you do to improve his oxygenation?
What other changes should you consider making in the ventilator settings?
If his oxygen saturation fails to improve despite being on high levels of support (eg. FIO2 of 1.0 and 20 cm H2O of PEEP), what other options do you have for improving his oxygenation
UW School of Medicine : School of Medicine Mission
Copyright and Disclaimer : Credits and Acknowledgements